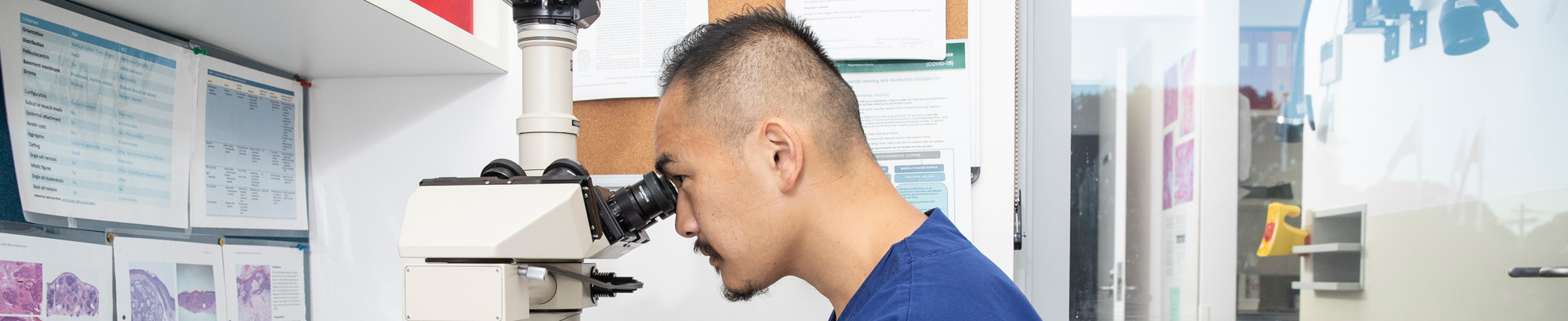
Mohs Surgery
With the Mohs technique for skin cancer treatment, Mohs Surgeons can precisely identify and remove an entire tumour while leaving the surrounding healthy tissue intact and undamaged. Mohs surgery (also known as microscopically controlled serial excision) offers the highest potential cure rates – even if the skin cancer has been previously treated by another method, while preserving cosmetic appearance as much as possible.
To ensure your skin cancer treatment will be performed with the highest standards of quality and competency, the Australasian College of Dermatologists accredited Mohs Surgeons have completed at least one year of supervised training and hands on experience provided by the Mohs surgeons at Oxford Day Surgery.
Overview
In the early 1940’s, Dr Frederick Mohs, Professor of Surgery at the University of Wisconsin, developed a new technique for the treatment of skin cancer: micrographic, margin-controlled surgery
This surgical technique is associated with the highest cure rates for multiple different skin cancers, such as basal and squamous cell carcinomas on the face. The tumor is surgically removed, processed and the excision margins microscopically evaluated whilst the patient waits. Using careful mapping techniques, the Dermatologist may need to return to the patient to remove any remaining tumor.This process is repeated until no cancer remains. The tumor is completely removed with minimal loss of normal skin. The cure rate is approximately 98-99% for primary tumors. As with conventional excision techniques, a direct closure, skin flap or skin graft may be required to close the final wound.
When is Mohs surgery recommended?
Mohs surgery is appropriate in the following situations:
- Tumors located atdifficult sites such as the head and neck, (especially around the nose, eyes, lips and ears), digits and genital areas
- A skin cancer that has recurred after previous treatment
- The skin cancer has an aggressive pattern of growth
- Tumors with poorly defined borders
- When dealing with tumors at a high-risk of local recurrence or spread
- Where tissue conservation is paramount
The major advantages of Mohs' Surgery are:
The tumor is completely removed with minimal loss of normal skin
The rate of cure for primary tumors is approximately 98-99%, which is substantially higher than any other method of treatment, including conventional excisional surgery
The Procedure
- Treatment is performed under local anesthetic.
- In selected cases sedation may be used, either through oral medication, or very rarely, by injection.
- The visible tumor, together with a small margin of visually normal skin is removed; this is known as a “first-stage”. Bleeding is controlled and a pressure dressing is then applied, and the patient is taken to wait in a comfortable, private recovery area while the slides are being processed. The first-stage will take approximately 10-15 minutes.
- The removed tissue is carefully divided into pieces that will sit on a microscopic slide. The edges are then marked with specially colored dyes; a careful map is made of the tissue removed, and the tissue is frozen by the technician. Thin slices can then be made from the frozen tissue and examined microscopically by the doctor who is now able to visualize any residual cancer. (This process can take up to 1 hour)
- If cancer cells remain, another layer of tissue is then surgically removed (another “Stage”), and theprocedure is repeated until no cancer cells remain at the surgical margins.
- This overall process can take between 1 to 4 hours, depending on the extent of the cancer, the number of stages required, and the laboratory processing time required to clear all of the tumor present.
What happens after the tumor has been removed?
After Mohs Surgery, a surgical wound, or defect, will be left. This wound can be managedin several ways. The options will be discussed with the patient in order to provide the best possible functional and cosmetic results.
The reconstructive options include
- Direct closure of the wound, or part of the wound, with sutures
- Skin flaps, skin grafts, or combinations of these techniques
- Healing by spontaneous granulation
- Referral for reconstruction